Biologic width is a critical concept in restorative dentistry, impacting both the long-term health and esthetics of dental restorations. CONDUCT.EDU.VN offers this comprehensive guide that explores the definition, clinical significance, and management of this essential anatomical dimension. Understanding connective tissue attachment, epithelial attachment, and the implications of violating the biological imperative helps clinicians achieve predictable and lasting results.
1. Understanding Biologic Width: Definition and Historical Context
Biologic width refers to the dimension of the soft tissue attachment to the tooth, comprising the connective tissue and epithelial attachments. This zone is crucial for maintaining gingival health and stability around teeth and dental implants. Understanding the historical context and evolution of this concept is fundamental for dental professionals.
1.1 The Original Research: Garguilo, Wentz, and Orban’s Contribution
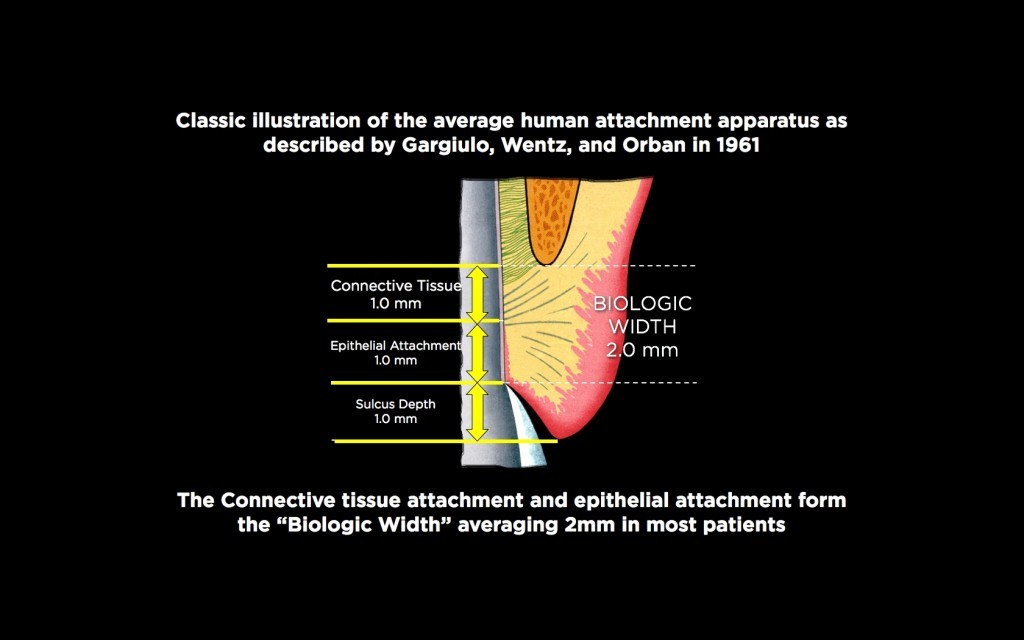
In 1961, Garguilo, Wentz, and Orban published a landmark study based on cadaver specimens that detailed the dimensions of the dentogingival junction. They determined that, on average, the connective tissue attachment measured approximately 1 mm, and the epithelial attachment also measured around 1 mm. This led to the widely cited figure of 2 mm for biologic width. They also noted an average facial sulcus depth of 1 mm, resulting in a total gingival height of about 3 mm above the bone on the facial aspect.
1.2 The Evolution of the Term: Dr. D. Walter Cohen
Interestingly, Garguilo, Wentz, and Orban did not use the term “biologic width” in their original 1961 publication. The term was coined in 1962 by Dr. D. Walter Cohen at the University of Pennsylvania, solidifying its place in dental terminology.
1.3 Individual Variation: Vacek’s Cadaver Studies
Further research by Vacek in 1994, also using cadaver studies, revealed important insights into the clinical variability of biologic width. Vacek confirmed the average biologic width of 2 mm but emphasized that this dimension varies significantly among individuals. Some individuals may have a biologic width as small as 0.75 mm, while others may have one as large as 4 mm. However, the majority of the population tends to adhere to the 2 mm average. Vacek also found that biologic width was relatively consistent across all teeth within the same individual.
2. Clinical Significance of Biologic Width
The primary clinical importance of biologic width lies in its relationship to restorative margin placement and its influence on post-surgical tissue stability. Violating the integrity of the connective tissue attachment or epithelial attachment can lead to several adverse outcomes.
2.1 Implications of Biologic Width Violation
When a restorative margin is placed too close to the alveolar bone, invading the biologic width, two common responses can occur:
- Bone Resorption: The body may attempt to recreate the necessary space for the biologic width by resorbing the alveolar bone. This is a typical response seen around dental implants, resulting in a characteristic “funnel” of bone loss around the implant neck, extending to the first thread.
- Gingival Inflammation: Around natural teeth, the most frequent response to biologic width encroachment is gingival inflammation. This inflammation can manifest as redness, swelling, bleeding on probing, and discomfort. Chronic inflammation can also contribute to periodontal disease progression.
2.2 Biologic Width and Post-Surgical Tissue Response
Following surgical procedures such as crown lengthening or gingivectomies, the biologic width will reform through coronal migration of the gingival tissues. This migration aims to re-establish both the appropriate biologic width dimension and a normal sulcus depth. If the surgical plan does not adequately consider the patient’s biologic width dimensions, the final gingival position may be unstable, leading to coronal migration of the gingiva and potential compromise of the restoration.
2.3 Consequences of Ignoring Biologic Width
Failure to respect the biologic width can result in:
- Chronic gingival inflammation and discomfort.
- Unpredictable tissue response following restorative or surgical procedures.
- Compromised esthetics due to inflammation or recession.
- Accelerated periodontal disease progression.
- Increased risk of restoration failure.
3. Restorative Margin Placement and Biologic Width
The placement of restorative margins is a critical decision that directly affects the health and longevity of dental restorations. Understanding the relationship between margin placement and biologic width is essential for preventing complications.
3.1 Supra-Gingival vs. Sub-Gingival Margins
The first decision to make when planning restorative margin placement is whether the margin can be placed supra-gingival (above the gingival margin), equigingival (at the gingival margin), or sub-gingival (below the gingival margin).
- Supra-gingival and Equigingival Margins: When possible, placing margins supra-gingival or equigingival is preferred. This approach avoids the potential for biologic width violation, assuming the gingiva is healthy and mature. With the advent of highly esthetic translucent materials like lithium disilicate, it is often possible to achieve excellent esthetic results without the need for subgingival margin placement.
- Sub-Gingival Margins: There are situations where subgingival margin placement is necessary. Indications for subgingival margins include:
- Structural issues, such as caries extending below the gingival margin.
- Cervical erosion or abfraction lesions.
- The presence of old restorations requiring extension.
- The need to extend the restoration for ferrule.
- Significant tooth discoloration requiring masking with a more opaque restorative material like zirconia or metal-ceramic.
3.2 The “2.5 mm Rule” and Its Limitations
Historically, a common guideline for subgingival margin placement was to place the margin 2.5 mm from the alveolar bone. This was based on the assumption that the biologic width was a constant 2 mm (as described by Garguilo), and an additional 0.5 mm was added for safety.
However, as Vacek’s research demonstrated, biologic width varies among individuals. Therefore, the “2.5 mm rule” can be problematic. In patients with a biologic width greater than 2 mm, this rule could lead to a violation. In patients with a smaller biologic width, the margin might be unnecessarily deep.
3.3 Ideal Subgingival Margin Placement
The ideal location for a subgingival margin is within the gingival sulcus, above the epithelial attachment. In other words, the margin should be below the free gingival margin but not impinging on the connective tissue or epithelial attachments.
The challenge is determining the location of the epithelial attachment in each individual patient. While probing to bone can provide an indication, it does not directly measure the biologic width. Accurate determination requires careful clinical judgment and consideration of individual patient factors.
3.4 The Importance of Individualized Assessment
When placing subgingival margins, it is essential to assess each patient individually. Factors to consider include:
- Gingival Biotype: Thick, fibrotic gingiva is more resistant to recession than thin, scalloped gingiva.
- Sulcus Depth: The depth of the gingival sulcus provides an indication of the amount of unattached gingiva.
- Probing Depths: Probing depths can help identify areas of inflammation or potential biologic width violation.
- Radiographic Assessment: Radiographs can help assess the proximity of the restorative margin to the alveolar bone.
- Patient History: A history of previous restorations, periodontal disease, or gingival recession can provide valuable information.
4. Understanding Gingival Presentations and Their Impact
Different gingival presentations require tailored approaches to subgingival margin placement. Recognizing these variations is crucial for achieving predictable outcomes and minimizing complications.
4.1 Probing the Facial Sulcus
Before placing a subgingival margin, it is essential to carefully probe the facial sulcus of the tooth. It’s important to remember that the probe typically penetrates the epithelial attachment by approximately 0.5 mm, meaning the actual sulcus depth is usually 0.5 mm less than the probed depth. In cases of gingival inflammation, the probe may penetrate even deeper into the attachment.
4.2 Normal or Shallow Sulcus Depths (1 mm to 1.5 mm)
In patients with normal or shallow facial sulcus depths (typically 1 mm to 1.5 mm), the primary risk associated with subgingival margin placement is violating the biologic width by placing the margin too deep. The histologic sulcus depth is likely less than 1 mm in these cases, making it easier to impinge on the epithelial or connective tissue attachments.
The advantage of this presentation is that these patients are generally at lower risk of gingival recession following restoration. The gingival dimension above the bone is commonly around 3 mm on the facial aspect, meaning that significant bone loss would need to occur for the tissue to recede apically and expose the margin.
In these patients, it’s unnecessary to place the margin more than 0.5 mm to 0.7 mm below the tissue. This placement is typically sufficient to hide the margin visually without violating the attachment or increasing the risk of future recession.
4.3 Deeper Facial Sulcus Depths (2 mm to 4 mm or More)
Patients with deeper facial sulcus depths (2 mm to 4 mm or more) present a different set of challenges. These patients are at a higher risk of gingival recession following restoration unless the margin is placed further below the tissue.
The increased risk of recession is due to the presence of several millimeters of unattached gingiva above the biologic width. The thickness of this unattached tissue also influences the risk; thinner tissue and deeper sulcus depths are associated with a greater likelihood of recession.
The advantage of this presentation is that it is more difficult to violate the biologic width in these patients. The margin would need to be placed 2 mm to 4 mm below the gingiva to reach the attachment.
5. Subgingival Margin Placement Techniques
Achieving precise subgingival margin placement requires careful technique and attention to detail. Here are some specific methods for managing different clinical scenarios.
5.1 Subgingival Margin Placement in Shallow Sulcus Patients (Less Than 1.5 mm)
In patients with sulcus depths less than 1.5 mm, the goal is to place the margin 0.5 mm to 0.7 mm below the tissue. This protects the attachment while ensuring the margin remains covered by gingiva. Because the risk of recession is low, this placement typically provides excellent esthetics and long-term stability.
Step-by-Step Technique:
-
Tooth Preparation: Prepare the tooth completely, extending the preparation to the existing gingival margin level. Leave only the final subgingival margin placement to be completed.
-
Sulcus Probing: Probe the sulcus to confirm that the probing depth is 1.5 mm or less.
-
Retraction Cord Placement: Place an appropriately sized retraction cord (e.g., Ultradent Ultrapak cord #00 for thin tissue or #1 for most tissue) into the sulcus. The key is to place the cord 0.5 mm to 0.7 mm apical to the prepared margin, which was left at the height of the gingival margin. Dampen the cord with an aluminum chloride solution.
-
Final Margin Preparation: Use a bur that provides adequate depth and shape for your finish line to prepare to the top of the cord. The first cord retracts the tissue and represents the correct position for the final prep margin, 0.5 mm to 0.7 mm subgingival.
-
Second Cord Placement: Place a second layer of cord, pushing it apically so it sits at the level of the prepped margin. Ensure that you can visualize the second cord all around the tooth. If you cannot see the second cord, it has been placed too deep.
-
Impression: Wet the top cord with water, remove it, air dry the sulcus, and take your impression, either traditionally or optically.
-
Restoration Placement: Place the completed restoration, ensuring proper fit and contour.
5.2 Margin Placement for Deep Sulcus Patients (Greater Than 2 mm)
Managing patients with deeper facial probing depths (greater than 2 mm) requires a different approach. The primary challenge is the risk of future recession due to the amount of unattached tissue present above the biologic width.
The first step is to determine the reason for the deep sulcus depth, which typically falls into one of two categories:
-
Altered Passive Eruption: The gingiva has not receded to a normal position relative to the bone and cementoenamel junction (CEJ). This is characterized by teeth that appear to have short clinical crown lengths.
-
Bone Loss Without Recession: The attachment has migrated apically with bone loss, but the gingiva has not followed, creating a pocket formation. In these patients, the clinical crown lengths are typically normal.
5.2.1 Altered Passive Eruption
In cases of altered passive eruption, a gingivectomy can be performed to eliminate the deep sulcus and improve the length of the clinical crowns. However, it is essential to perform the gingivectomy across all the anterior teeth to ensure that the gingival levels flow correctly from canine to lateral to central incisor.
When performing a gingivectomy, it is crucial not to remove so much gingiva that the remaining sulcus is less than 1 mm in depth. Otherwise, the tissue will simply grow back.
5.2.2 Bone Loss Without Recession
In patients with bone loss without recession, a gingivectomy is not typically indicated, as it would result in excessively long and narrow clinical crowns. These patients are generally at greater risk of recession following restoration.
5.3 General Guidelines for Deep Sulcus Patients
When restoring anterior teeth with facial probing depths greater than 2 mm, consider the following guidelines:
- Supragingival Margin Placement: If possible, place the margin supragingival. This is readily achievable with translucent all-ceramic materials, especially if the existing tooth color is acceptable. A supragingival margin minimizes trauma to the gingiva and reduces the risk of future recession.
- Subgingival Margin Placement: If a subgingival margin is necessary due to tooth discoloration or the need for a more opaque restorative material, place the margin at half the depth of the probing. For example, for a 3 mm facial sulcus depth, place the margin 1.5 mm below the tissue. This approach minimizes the risk of margin exposure if some recession occurs.
6. Diagnosing and Managing Biologic Width Violations
Recognizing the signs and symptoms of a biologic width violation is crucial for effective treatment. Early diagnosis and management can prevent further complications and ensure the long-term success of dental restorations.
6.1 Signs and Symptoms of Biologic Width Violation
When an anterior restoration, particularly a full crown, exhibits significant gingival inflammation, consider the following possible diagnoses:
- Plaque Control Issues: Unlikely if adjacent teeth have healthy gingiva.
- Marginal Fit Problems: Examine with an explorer and radiograph.
- Poor Contour: Can prevent adequate hygiene.
- Allergic Response: Especially if the restoration was done in the ’80s or ’90s using a nickel-containing alloy and the patient is female.
- Biologic Width Violation: The margin is placed too close to bone.
6.2 Diagnostic Techniques
- Temporary Restoration: Remove the existing restoration and place a well-fitting temporary for at least three months. If the gingival inflammation resolves and does not return, the margin location was likely the problem. However, it is important to wait the full three months, as inflammation can sometimes reappear after the tissue has healed and matured (typically 8 to 12 weeks).
- Probing: Place a periodontal probe in the sulcus until it reaches the margin, circumferentially around the tooth. A margin in the sulcus will result in no pain, while a margin in the connective tissue attachment will be painful to probe.
- Anesthesia and Probing to Bone: Anesthetize the tooth. Place the periodontal probe on the restorative margin and measure the distance to the gingival margin. Keeping the probe against the root laterally, slide the probe down to bone, allowing you to compare the previous probe readings with the distance to bone.
- Radiographs: Use a periapical radiograph to assess the margin location relative to bone on the interproximal.
If the margin is painful to probe, is within 2 mm of the bone when measuring, or appears to violate the biologic width on a radiograph, a biologic width violation is likely present.
6.3 Treatment Options for Biologic Width Violations
The only way to eliminate inflammation caused by a biologic width violation is to either move the margin away from the bone or move the bone away from the margin.
-
Moving the Margin:
- Orthodontic Extrusion: Move the tooth coronally, bringing the margin with it.
- Root Reshaping: Smooth away the old margin and prepare a new margin at a more coronal and correct level. This is most useful when the previous tooth preparation involved minimal tooth reduction.
-
Moving the Bone:
- Osseous Surgery: Remove bone to increase the distance between the margin and the bone. This is the most common solution for biologic width violations, but it carries the risk of recession.
6.4 Surgical Correction of Facial Biologic Width Violations
For single central incisors with a biologic width violation on the facial surface, osseous surgery is often the preferred approach. A facial flap is elevated, the necessary facial bone is removed, and the flap is replaced to its original position. If the tissue is of normal thickness, recession is rare. If the tissue is thin, the risk of recession is higher, but a connective tissue graft can be used to cover the root and margin if necessary.
6.5 Managing Interproximal Biologic Width Violations
Osseous surgery is rarely indicated for correcting an interproximal biologic width violation on a single anterior tooth because it requires removal of interproximal bone, which is followed by a loss of papilla height and an open embrasure.
Instead, the ideal treatment to expose adequate tooth structure for restoration and allow for ideal esthetics with no loss of interproximal papilla height is orthodontic extrusion.
6.6 Orthodontic Extrusion Techniques
There are two ways to accomplish orthodontic extrusion:
- Slow Extrusion: Extrude the tooth 0.5 mm to 1 mm per month, allowing the bone and gingiva to follow the tooth. This is then followed by osseous surgery to reposition the bone and gingiva ideally, which exposes the tooth as well. This approach is highly predictable and is generally chosen, especially when there are other orthodontic concerns.
- Rapid Extrusion: Perform all of the movement within four weeks. The key to this approach is to perform supracrestal fiberotomies weekly to discourage the bone and gingiva from following. It is necessary to retain the tooth in position for at least 12 more weeks to prevent re-intrusion and to evaluate if osseous surgery is necessary due to the bone and gingiva creeping in a coronal direction.
In all cases where forced extrusion is being used to resolve a biologic width violation, the amount of root in bone is being reduced by the amount the tooth is being extruded. While clinicians often worry about keeping a 1:1 crown-to-root ratio at a minimum, experience has shown that leaving 8 mm to 9 mm of root in bone has provided a successful long-term solution.
7. Managing Biologic Width Violations on Multiple Adjacent Teeth
Patients with multiple adjacent existing anterior crowns, prepped essentially to bone, are some of the most challenging esthetic cases to treat. There is usually significant gingival inflammation, and if the crowns were bonded, there is often significant black staining from the bacterial growth that occurs when attempting to bond in a highly contaminated environment.
The only successful solution is to start by addressing the biologic width problem first by correcting the bone-to-margin distance with osseous surgery. Bone removal creates a risk of recession, especially when bone has to be removed on both the facial and interproximal.
7.1 Treatment Steps
-
Remove Old Crowns: Remove the old crowns to visualize the quality of each tooth and assess the distance from the margin to bone using a probe 360 degrees around the tooth. This also allows you to see how heavy the prior tooth reduction was and if the reduction at the margin was minimal.
-
Root Reshaping (If Possible): With a slice-type finish line, it is often possible to do minor “root reshaping” by essentially smoothing out the old margin. This needs to be followed by re-prepping a new margin the correct distance from bone, which eliminates the need for bone removal.
-
Osseous Surgery (If Necessary): When the preps are heavy shoulders or chamfers, bone removal becomes mandatory. The amount of bone removal is dictated by how close the existing margins are to the bone and whether all the teeth were prepped the same or not. Move the bone 2.5 mm to 3 mm away from the existing margins all the way around the teeth to accommodate the biologic width.
-
Suturing: At the time of suturing, assuming the pre-treatment crown length was acceptable (i.e., no crown lengthening was desired), the flap should be replaced exactly where it was pre-surgically, not apically positioned. The goal is to hope for a longer attachment apparatus rather than a deeper pocket followed by recession.
-
Healing Period: Wait at least six months before moving forward. This allows adequate time for healing and maturation of the tissues.
Depending upon the patient’s gingival thickness, it can be surprising how often no recession occurs on either the facial or interproximal, even when 2 mm of bone has been removed around the teeth.
8. FAQ: Addressing Common Questions About Biologic Width
Here are some frequently asked questions about biologic width and its clinical implications:
- What happens if biologic width is violated? Violation can lead to gingival inflammation, bone loss, and potential restoration failure.
- How can I accurately measure biologic width? While direct measurement is not possible clinically, careful probing, radiographic assessment, and consideration of individual factors can help estimate its dimension.
- Is there a “safe” distance for placing subgingival margins? Not a universal one. Individualized assessment is key, considering gingival biotype, sulcus depth, and probing depths.
- Can biologic width violations be prevented? Yes, by carefully planning restorative procedures and considering individual patient factors.
- What materials are best for restorations near the gingiva? Highly esthetic translucent materials like lithium disilicate are preferred to avoid the need for deep subgingival margins.
- How does periodontal disease affect biologic width? Periodontal disease can lead to apical migration, altering its dimensions and requiring careful management.
- Is biologic width important for dental implants? Yes, a similar concept exists around implants, requiring adequate space for soft tissue attachment.
- What is the role of crown lengthening in managing biologic width? Crown lengthening can be used to increase the distance between the margin and bone in cases of violation.
- Can biologic width violations cause pain? Yes, inflammation can lead to pain and discomfort.
- How often should biologic width be assessed? It should be considered during the planning phase of any restorative or surgical procedure involving the gingiva.
9. Conclusion: Prioritizing Biologic Width for Long-Term Success
Understanding and respecting biologic width is essential for achieving predictable and long-lasting results in restorative dentistry. By carefully considering individual patient factors, employing appropriate techniques for margin placement, and promptly addressing any violations, dental professionals can help ensure the health, stability, and esthetics of dental restorations.
For more detailed information and guidance on biologic width and other essential dental concepts, visit CONDUCT.EDU.VN. Our comprehensive resources are designed to help you provide the highest quality care for your patients.
Are you struggling to find reliable information about dental regulations? Do you feel overwhelmed by the complexities of clinical compliance? conduct.edu.vn can help! Visit our website today to explore our extensive collection of articles, guides, and resources designed to simplify compliance and enhance your understanding of ethical dental practices. Contact us at 100 Ethics Plaza, Guideline City, CA 90210, United States or Whatsapp: +1 (707) 555-1234.