Vaccinology: A guide to vaccine development and application from the basic science to new advancements is essential for understanding how vaccines protect individuals and populations. CONDUCT.EDU.VN offers in-depth knowledge of immunological memory, herd immunity, and non-specific effects, providing clarity on the multifaceted benefits of vaccination. This guide will help you grasp crucial concepts such as vaccine-induced protection, infection prevention, and the significance of immunological advancements.
1. Understanding Immune Memory in Vaccinology
Immune memory is a cornerstone of vaccine-induced protection. When an individual encounters a pathogen, their immune system, if previously vaccinated against that specific pathogen, can mount a protective immune response more rapidly and robustly. Immune memory is sufficient for protection when the incubation period is long enough for a new immune response to develop.
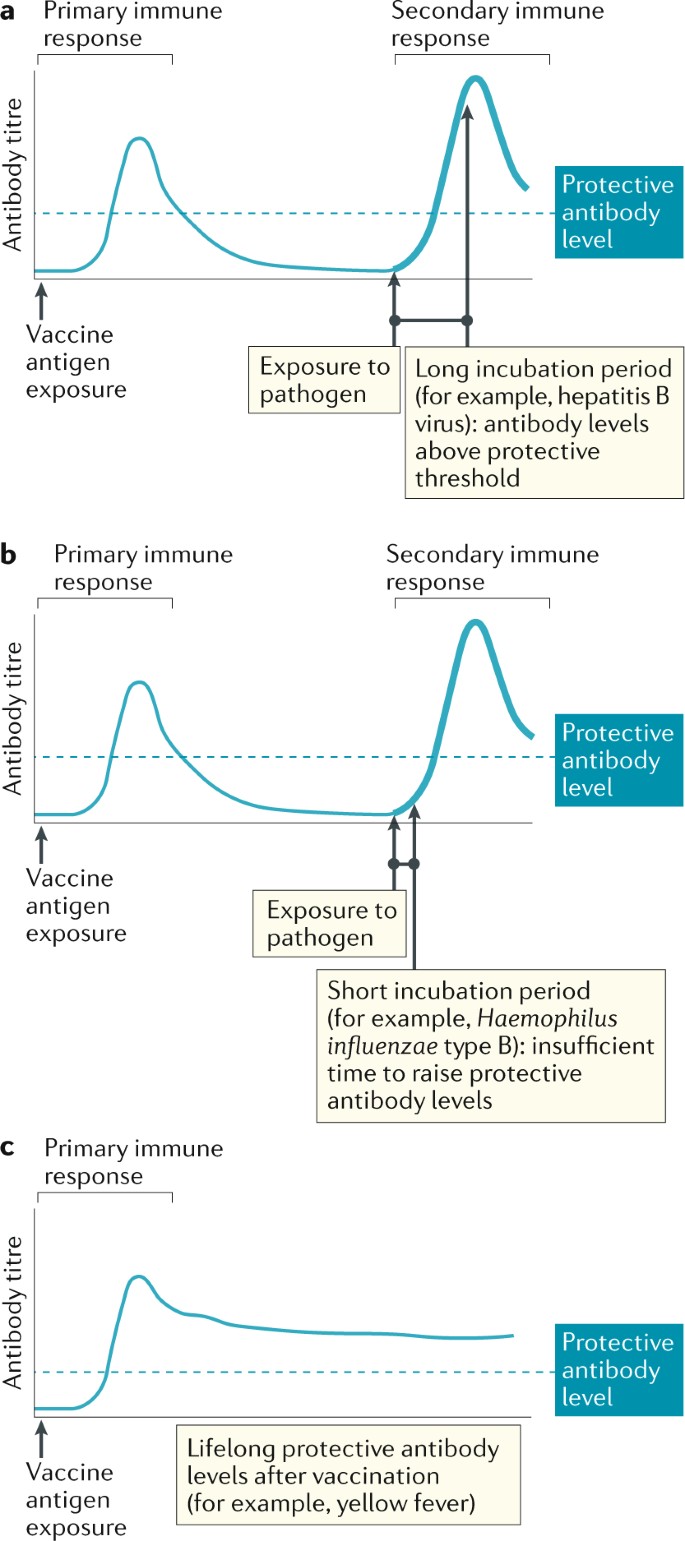 Immune memory allows a faster and stronger response to known pathogens
Immune memory allows a faster and stronger response to known pathogens
1.1. The Dynamics of Immune Memory
The success of immune memory depends on several factors:
- Incubation Time: For infections with long incubation periods, like Hepatitis B (HBV), immune memory is highly effective. HBV has an incubation period of 6 weeks to 6 months, allowing the vaccinated individual ample time to mount a protective response.
- Quality of Memory Response: The effectiveness of the memory response, which is determined by the type and number of immune cells available.
- Antibody Levels: The level of antibodies produced by memory B cells.
- Waning Antibody Levels: Antibody levels in the circulation wane after primary vaccination, often falling below the level required for protection.
1.2. Limitations of Immune Memory
Immune memory may not be sufficient for protection against rapidly invasive bacterial infections that can cause severe disease within hours or days. Examples include Haemophilus influenzae type B (Hib) and capsular group C meningococcal infection. Individuals with vaccine-induced immune memory can still develop disease once their antibody levels have waned, despite mounting robust, although not rapid enough, memory responses.
The waning of antibody levels varies depending on:
- Age of the Vaccine Recipient: Waning is very rapid in infants because of the lack of bone marrow niches for B cell survival.
- Nature of the Antigen: Virus-like particles in the HPV vaccine induce antibody responses that can persist for decades, whereas pertussis vaccines induce relatively short-term antibody responses.
- Number of Booster Doses Administered: Multiple booster doses can sustain antibody levels above the protective threshold.
1.3. Strategies to Enhance Immune Memory
To sustain immunity, booster doses of vaccines are administered throughout childhood, as is the case for diphtheria, tetanus, pertussis, and polio vaccines. For example, five or six doses of tetanus or diphtheria vaccine in childhood provide lifelong protection, and booster doses of these vaccines throughout adult life are not routine in most countries that can achieve high coverage with multiple childhood doses.
Lifelong protection is typical following a single dose with some live attenuated viral vaccines, such as the yellow fever vaccine. However, protection is incomplete with others. Breakthrough cases can occur during disease outbreaks among those vaccinated against varicella zoster and measles-mumps, though these cases are usually mild in individuals who have had two doses of the measles-mumps-rubella vaccine or varicella zoster vaccine.
1.4. The Concept of Original Antigenic Sin
The complexity of immune memory is illustrated by the concept of ‘original antigenic sin’. This phenomenon describes how the immune system fails to generate an effective immune response against a new strain of a pathogen if the host was previously exposed to a closely related strain. This has been demonstrated in infections such as dengue and influenza.
Strategies to overcome original antigenic sin include:
- Using adjuvants that stimulate innate immune responses, inducing sufficiently cross-reactive B cells and T cells that recognize different strains.
- Including as many strains as possible in a vaccine.
CONDUCT.EDU.VN provides comprehensive resources to understand and navigate the complexities of vaccine-induced immune responses.
2. The Significance of Herd Immunity in Vaccinology
Herd immunity, more correctly termed ‘herd protection,’ is a critical component of vaccine-induced protection. Vaccines cannot directly protect every individual in a population, as some individuals are not vaccinated for various reasons, and others do not mount an immune response despite vaccination. If enough individuals in a population are vaccinated, transmission of the pathogen can be interrupted, and the incidence of disease can fall further than expected.
2.1. How Herd Immunity Works
Herd immunity protects individuals who are susceptible because they:
- Have not yet been immunized (e.g., being too young).
- Cannot be immunized (e.g., as a result of immunodeficiency).
- Did not develop immunity from the vaccine.
- Experienced waning immunity.
- Refused immunization.
2.2. Vaccination Coverage Thresholds
For highly transmissible pathogens, such as those causing measles or pertussis, approximately 95% of the population must be vaccinated to prevent disease outbreaks. For less transmissible organisms like polio, rubella, mumps, or diphtheria, vaccine coverage can be ≤86%. For influenza, the threshold for herd immunity varies from season to season and is influenced by vaccine effectiveness. Modest vaccine coverage of 30–40% can impact seasonal influenza epidemics, but ≥80% coverage is optimal.
2.3. Potential Downsides of High Vaccination Rates
There might be a downside to very high vaccination rates. The absence of pathogen transmission will prevent natural boosting of vaccinated individuals, leading to waning immunity if booster doses are not used. Apart from the tetanus vaccine, all other vaccines in the routine immunization schedule induce some degree of herd immunity, substantially enhancing population protection beyond that achieved by individual vaccination.
2.4. Examples of Successful Herd Immunity
- Meningococcal Vaccine: Vaccination of children and young adults with capsular group C meningococcal vaccine in a mass campaign in 1999 resulted in almost complete elimination of disease from the UK in adults and children. The strategy for controlling capsular groups A, C, W, and Y meningococci in the UK involves vaccinating adolescents, as they are mainly responsible for transmission, leading to community protection.
- HPV Vaccine: Initially introduced to control HPV-induced cervical cancer with programs directed at girls, the HPV vaccine also provides protection against HPV infection in heterosexual boys through herd immunity, leading to a marked reduction in the total HPV burden in the population.
CONDUCT.EDU.VN highlights the importance of herd immunity in achieving comprehensive public health outcomes through vaccination.
3. Prevention of Infection Versus Disease in Vaccinology
Whether vaccines prevent infection or, rather, the development of disease after infection with a pathogen is often difficult to establish, but improved understanding of this distinction could have significant implications for vaccine design.
3.1. BCG Vaccine: An Illustrative Example
The BCG vaccine provides an example of how vaccines can prevent both disease and infection. It prevents severe disease manifestations such as tuberculous meningitis and miliary TB in children. Animal studies have shown that BCG vaccination reduces the spread of M. tuberculosis bacteria in the blood, mediated by T cell immunity, thereby protecting against the development of disease after infection.
3.2. Evidence for Infection Prevention
BCG vaccination also reduces the risk of infection. In a TB outbreak at a school in the UK, 29% of previously BCG-vaccinated children had a memory T cell response to infection, as indicated by a positive interferon-γ release assay, compared with 47% of the unvaccinated children. A similar effect was seen when studying Indonesian household members of patients with TB, who had a 45% reduced chance of developing a positive interferon-γ release assay response to M. tuberculosis if they had previously been BCG vaccinated.
The lack of a T cell response in previously vaccinated individuals indicates that the BCG vaccine induces an innate immune response that results in ‘early clearance’ of the bacteria, preventing infection that induces an adaptive immune response. Understanding the induction of such protective innate immune responses is valuable for future vaccine development.
3.3. Implications for SARS-CoV-2 Vaccines
In the case of the current SARS-CoV-2 pandemic, a vaccine that prevents severe disease and disease-driven hospitalization can have a substantial public health impact. A vaccine that also blocks virus acquisition and prevents asymptomatic and mild infection would have a much larger impact by reducing community transmission and potentially establishing herd immunity.
CONDUCT.EDU.VN emphasizes the dual role of vaccines in preventing infection and disease, underscoring the need for advanced vaccine designs that offer comprehensive protection.
4. Exploring Non-Specific Effects of Vaccines in Vaccinology
Immunization with some vaccines perturbs the immune system, resulting in general changes in immune responsiveness that can increase protection against unrelated pathogens. This phenomenon is best described in humans in relation to BCG and measles vaccines.
4.1. Mortality Reductions
Studies have shown marked reductions in all-cause mortality when BCG and measles vaccines are administered to young children, far beyond the expected impact from the reduction in deaths attributed to TB or measles. These non-specific effects may be particularly important in high-mortality settings, though not all studies have identified the phenomenon.
4.2. Proposed Immunological Mechanisms
The most plausible immunological mechanism is that epigenetic changes can occur in innate immune cells as a result of vaccination. However, there are no definitive studies in humans that link immunological changes after immunization with important clinical endpoints. It remains unclear how current immunization schedules might be adapted to improve population protection through non-specific effects.
4.3. The Shadow of Measles Disease
Recent studies have indicated that measles disease casts a prolonged ‘shadow’ over the immune system, depleting existing immune memory. Children who have had the disease have an increased risk of death from other causes over the next few years. In this situation, measles vaccination reduces mortality from measles as well as unconnected diseases that would have occurred during the ‘shadow’, resulting in a benefit that seems to be non-specific but actually relates directly to the prevention of measles disease and its consequences.
4.4. Limitations of Vaccine Study Protocols
Vaccine study protocols are usually designed to find pathogen-specific effects, and the possibility of important non-specific effects cannot be assessed.
CONDUCT.EDU.VN highlights the broader impacts of vaccination beyond specific disease prevention, advocating for a holistic understanding of vaccine benefits.
5. Key Considerations in Vaccine Development: Adjuvants and Delivery Systems
Modern vaccinology focuses on enhancing vaccine efficacy and safety through advanced adjuvants and delivery systems. These innovations aim to stimulate a more robust and targeted immune response, improving the overall effectiveness of vaccines.
5.1. The Role of Adjuvants
Adjuvants are substances added to vaccines to enhance the immune response. They work by:
- Prolonging Antigen Exposure: Slowing down the release of the antigen, allowing immune cells more time to respond.
- Activating Innate Immune Cells: Stimulating the innate immune system, which in turn activates adaptive immune responses.
- Improving Antigen Presentation: Enhancing the presentation of antigens to immune cells, leading to a stronger immune response.
Common adjuvants include aluminum salts, oil-in-water emulsions, and Toll-like receptor (TLR) agonists. The choice of adjuvant depends on the type of vaccine and the desired immune response.
5.2. Advanced Delivery Systems
Advanced delivery systems are designed to improve the targeting and uptake of vaccines by immune cells. These systems include:
- Liposomes: Spherical vesicles composed of lipid bilayers that can encapsulate antigens and deliver them to cells.
- Nanoparticles: Tiny particles that can be engineered to deliver antigens to specific immune cells, such as dendritic cells.
- Viral Vectors: Modified viruses that can deliver genetic material encoding antigens into cells, stimulating both humoral and cellular immunity.
5.3. mRNA Vaccines
mRNA vaccines represent a cutting-edge approach to vaccine development. These vaccines contain messenger RNA (mRNA) that encodes for a specific antigen. Once injected, the mRNA is taken up by cells, which then produce the antigen, stimulating an immune response. mRNA vaccines offer several advantages:
- Rapid Development: They can be developed quickly, making them suitable for responding to emerging infectious diseases.
- High Efficacy: They can elicit strong immune responses.
- Safety: They do not contain live pathogens, reducing the risk of infection.
5.4. Challenges and Future Directions
Despite advancements, there are challenges in vaccine development:
- Ensuring Safety: Rigorous testing and monitoring are essential to ensure vaccines are safe.
- Addressing Vaccine Hesitancy: Effective communication and education are needed to address public concerns about vaccines.
- Improving Global Access: Efforts are needed to ensure vaccines are accessible to all populations, regardless of economic status.
CONDUCT.EDU.VN remains committed to providing accurate and up-to-date information on the latest developments in vaccinology.
6. Ethical Considerations in Vaccine Development and Distribution
Vaccine development and distribution raise numerous ethical considerations that must be carefully addressed to ensure equitable and just outcomes.
6.1. Informed Consent
Informed consent is a fundamental ethical principle in vaccine development. Participants in clinical trials must be fully informed about the risks and benefits of the vaccine and must freely consent to participate. Special considerations are needed for vulnerable populations, such as children and individuals with cognitive impairments.
6.2. Risk-Benefit Assessment
A thorough risk-benefit assessment is essential in vaccine development. The potential benefits of the vaccine must outweigh the potential risks. This assessment should consider the severity of the disease, the efficacy of the vaccine, and the potential for adverse events.
6.3. Equitable Access
Equitable access to vaccines is a critical ethical consideration. Vaccines should be distributed fairly, regardless of socioeconomic status, geographic location, or other factors. This requires international cooperation and coordination to ensure that all populations have access to life-saving vaccines.
6.4. Prioritization Strategies
During a pandemic or outbreak, when vaccine supplies are limited, prioritization strategies are needed to determine who should receive the vaccine first. Ethical frameworks for prioritization should consider factors such as:
- Risk of Exposure: Prioritizing healthcare workers and other essential personnel who are at high risk of exposure.
- Risk of Severe Disease: Prioritizing individuals who are at high risk of severe disease or death, such as the elderly and those with underlying health conditions.
- Potential for Transmission: Prioritizing individuals who are likely to transmit the disease to others, such as those who live in crowded settings.
6.5. Transparency and Communication
Transparency and effective communication are essential for building public trust in vaccines. Public health officials should communicate openly and honestly about the risks and benefits of vaccines, address public concerns, and provide accurate information to counter misinformation.
6.6. Addressing Vaccine Hesitancy
Vaccine hesitancy is a complex issue influenced by various factors, including misinformation, mistrust, and concerns about safety. Addressing vaccine hesitancy requires a multi-faceted approach that includes:
- Building Trust: Establishing trust between healthcare providers and patients.
- Providing Accurate Information: Providing clear, accurate information about vaccines.
- Addressing Concerns: Addressing specific concerns and misconceptions about vaccines.
- Engaging Communities: Engaging with communities to understand and address their concerns.
CONDUCT.EDU.VN is dedicated to providing ethical guidance and resources to navigate the complex ethical landscape of vaccine development and distribution.
7. The Future of Vaccinology: Innovations and Challenges
Vaccinology is a rapidly evolving field, with ongoing research and development aimed at improving vaccine efficacy, safety, and accessibility.
7.1. Next-Generation Vaccines
Next-generation vaccines are being developed using advanced technologies to enhance immune responses and provide broader protection against infectious diseases. These include:
- Multivalent Vaccines: Vaccines that contain multiple antigens from different strains or variants of a pathogen, providing broader protection.
- Universal Vaccines: Vaccines that elicit immune responses against conserved regions of a pathogen, providing protection against multiple strains or variants.
- Therapeutic Vaccines: Vaccines that are designed to treat existing diseases, such as cancer or chronic infections.
7.2. Personalized Vaccines
Personalized vaccines are tailored to an individual’s unique immune profile, potentially enhancing immune responses and reducing the risk of adverse events. This approach involves analyzing an individual’s genetic makeup and immune status to design a vaccine that is specifically suited to them.
7.3. Artificial Intelligence in Vaccine Development
Artificial intelligence (AI) is being used to accelerate vaccine development by:
- Identifying Potential Vaccine Targets: AI algorithms can analyze large datasets to identify potential vaccine targets, such as antigens that are highly conserved and elicit strong immune responses.
- Predicting Vaccine Efficacy: AI models can predict vaccine efficacy based on preclinical and clinical data, helping to optimize vaccine design and development.
- Accelerating Clinical Trials: AI can be used to streamline clinical trials, such as by identifying eligible participants and monitoring adverse events.
7.4. Global Challenges in Vaccinology
Despite advancements, there are ongoing challenges in vaccinology:
- Emerging Infectious Diseases: The emergence of new infectious diseases, such as SARS-CoV-2, poses a constant threat to global health security.
- Antimicrobial Resistance: The rise of antimicrobial resistance threatens the effectiveness of antibiotics, making vaccines even more important for preventing bacterial infections.
- Vaccine Hesitancy: Vaccine hesitancy remains a significant challenge, undermining efforts to achieve herd immunity and protect vulnerable populations.
- Global Vaccine Access: Ensuring equitable access to vaccines in low- and middle-income countries remains a critical priority.
CONDUCT.EDU.VN is committed to addressing these challenges and promoting the advancement of vaccinology through education, research, and advocacy.
8. Frequently Asked Questions (FAQ) about Vaccinology
Q1: What is vaccinology?
Vaccinology is the study and development of vaccines to provide immunity against infectious diseases.
Q2: How do vaccines work?
Vaccines work by stimulating the immune system to produce antibodies and memory cells that protect against specific pathogens.
Q3: What is herd immunity?
Herd immunity is the protection of a population from an infectious disease when a high percentage of individuals are immune, either through vaccination or prior infection.
Q4: Are vaccines safe?
Yes, vaccines undergo rigorous testing and monitoring to ensure they are safe and effective.
Q5: What are the common side effects of vaccines?
Common side effects include mild fever, soreness at the injection site, and fatigue, which typically resolve within a few days.
Q6: Can vaccines cause autism?
No, numerous scientific studies have shown that there is no link between vaccines and autism.
Q7: What is an adjuvant?
An adjuvant is a substance added to a vaccine to enhance the immune response.
Q8: What are mRNA vaccines?
mRNA vaccines use messenger RNA to instruct cells to produce antigens, stimulating an immune response.
Q9: How are vaccines developed?
Vaccine development involves identifying antigens, conducting preclinical and clinical trials, and manufacturing and distributing the vaccine.
Q10: Why is it important to get vaccinated?
Vaccination protects individuals from infectious diseases, prevents outbreaks, and contributes to herd immunity, safeguarding public health.
For more information on vaccinology and ethical conduct, visit CONDUCT.EDU.VN at 100 Ethics Plaza, Guideline City, CA 90210, United States, or contact us via Whatsapp at +1 (707) 555-1234. conduct.edu.vn is your trusted resource for comprehensive guidelines and resources on vaccinology and ethical conduct.