1. Understanding the Inflammatory Response in Musculoskeletal Conditions
The inflammatory response is the body’s natural defense mechanism against injury and infection. When trauma occurs, such as a sprain or strain, the body initiates a complex series of events to repair the damaged tissue. This process involves the release of various chemical mediators that increase blood flow to the injured area, leading to redness, warmth, swelling, and pain.
1.1 Key Components of the Inflammatory Response
The inflammatory response comprises several key components:
- Increased Blood Flow: Vasodilation occurs to deliver more blood, oxygen, and nutrients to the injured site.
- Leukocyte Infiltration: White blood cells migrate to the area to remove debris and fight infection.
- Edema Formation: Fluid accumulation leads to swelling, which can limit range of motion.
- Pain Activation: Nerve endings are stimulated by inflammatory mediators, causing pain.
Understanding these components is crucial for healthcare providers to develop effective treatment strategies. Anti-inflammatory interventions, such as corticosteroid injections, can help to modulate this response and alleviate symptoms. According to the National Institutes of Health (NIH), managing inflammation early can significantly improve patient outcomes and prevent chronic pain conditions.
2. Essential Corticosteroid Considerations for Effective Injections
Corticosteroids are powerful anti-inflammatory medications commonly used in joint and soft tissue injections. They work by suppressing the immune system and reducing the production of inflammatory mediators. However, their use requires careful consideration to maximize benefits and minimize potential side effects.
2.1 Selecting the Right Corticosteroid
Choosing the appropriate corticosteroid depends on several factors, including the desired onset and duration of action. Short-acting corticosteroids, such as betamethasone acetate, provide rapid relief but have a shorter duration. Long-acting corticosteroids, such as methylprednisolone acetate, take longer to take effect but offer prolonged relief.
| Corticosteroid | Onset | Duration | Solubility |
|---|---|---|---|
| Betamethasone Acetate | Rapid | Short | High |
| Methylprednisolone Acetate | Slower | Prolonged | Low |
2.2 Injection Site Selection and Sterile Technique
Proper injection site selection is essential to ensure accurate delivery of the medication and minimize the risk of complications. Healthcare providers should have a thorough understanding of musculoskeletal anatomy and use sterile technique to prevent infection. This includes:
- Skin Preparation: Cleaning the injection site with an antiseptic solution.
- Sterile Gloves: Wearing sterile gloves during the procedure.
- Needle Handling: Using a new, sterile needle for each injection.
2.3 Limiting Injection Frequency
To avoid potential adverse effects, such as cartilage damage and tendon rupture, the frequency of corticosteroid injections should be limited. Generally, no more than one injection every three to four months is recommended. A study published in the Journal of Bone and Joint Surgery found that repeated corticosteroid injections can lead to degenerative changes in joint tissues.
2.4 Managing Flare Reactions
Flare reactions, characterized by increased pain and swelling, can occur after corticosteroid injections. These reactions are often due to the crystallization of the steroid within the joint. Healthcare providers should educate patients about this possibility and provide strategies for managing symptoms, such as ice packs and oral pain medications.
3. Anesthetic Agents: Enhancing Comfort and Efficacy in Joint Injections
Anesthetic agents play a crucial role in joint and soft tissue injections by providing immediate pain relief and enhancing patient comfort. Selecting the appropriate anesthetic agent and understanding its properties are essential for a successful injection procedure.
3.1 Choosing the Right Anesthetic Agent
The choice of anesthetic agent depends on the desired onset and duration of action, as well as the patient’s allergy history. Lidocaine is a commonly used anesthetic agent that provides rapid pain relief, while bupivacaine offers a longer duration of action.
| Anesthetic Agent | Onset | Duration | Concentration |
|---|---|---|---|
| Lidocaine | Rapid | Short | 1% or 2% |
| Bupivacaine | Slower | Long | 0.25% or 0.5% |
3.2 Allergy Considerations
Before administering an anesthetic agent, healthcare providers must meticulously review and document the patient’s allergy history. Some patients may report allergies to specific anesthetics or preservatives. In such cases, alternative agents should be considered.
3.3 Avoiding Epinephrine in Joint Injections
Mixing epinephrine with an anesthetic agent is generally not recommended for joint injections. Epinephrine can cause constriction of the synovial lining, leading to increased pain.
3.4 Toxicity Awareness
Healthcare providers should be aware of the toxic ranges of anesthetic agents and consider factors such as age, medical conditions, and overall nutritional status when determining the appropriate dose. Patients with hepatic or cardiovascular disease require special attention, as they may be more susceptible to adverse effects.
4. Pre- and Post-Injection Considerations: Optimizing Patient Outcomes
Proper pre- and post-injection considerations are crucial for optimizing patient outcomes and minimizing the risk of complications. This includes a thorough patient evaluation, appropriate needle selection, sterile skin preparation, and comprehensive discharge instructions.
4.1 Thorough Patient Evaluation
Before performing an injection, healthcare providers should conduct a thorough physical examination and review the patient’s medical history. This helps to identify any contraindications or potential risk factors. Assessment of involved musculoskeletal structures may include radiographs or magnetic resonance imaging.
4.2 Needle Selection
The choice of needle depends on the intended injection site. Intra-articular injections require longer needles, while trigger-point injections necessitate shorter needles. Needle gauge should be appropriate for the viscosity of the injected solution.
| Injection Type | Needle Gauge | Needle Length |
|---|---|---|
| Intra-articular | 21-gauge | 1 ½- to 2-inch |
| Trigger-point | 25-gauge | ½-inch |
| Trochanteric Bursitis | 22-gauge | Spinal needle |
4.3 Sterile Skin Preparation
Sterile technique is essential to prevent infection. The skin should be prepped with an antiseptic solution, such as povidone-iodine or chlorhexidine. Sterile gloves should be worn during the procedure.
4.4 Discharge Instructions
Patients should receive comprehensive discharge instructions that outline the expected effects of the injection, potential side effects, and instructions for pain management. They should also be provided with a call-back phone number for any concerns.
Table 3. Discharge Instruction Example
| Corticosteroids are a class of medications related to cortisone – a steroid. Medications in this class of anti-inflammatory drugs are powerful and can reduce inflammation quickly. Corticosteroids are not pain medications but when they reduce inflammation, they can have a direct impact on pain relief. While the inflammation for which corticosteroids are given can recur, in most cases, patients experience relief of their symptoms for many months and possibly for years. Steroid injections are intended to relieve inflammation from conditions such as tendonitis, bursitis, arthritis, and painful spinal cord/nerve root conditions. Steroid injections should be limited to three to four times per year because of the potentially harmful changes seen in tissue/joint structures in patients who receive too many steroid injections. Side Effects – Flare Reaction – An unintended increase in pain or swelling following a corticosteroid injection. This can occur as a result of needle trauma to the joint or a crystallization of the steroid solution within the joint. This reaction usually resolves within 48 to 72 hours of onset. – Elevated Blood Sugar – Follow your primary care provider’s recommendations on blood sugar elevation. Check your blood sugar frequently over the next 3 days because it could rise as a result of your injection. – Facial Flushing – Pain – Infection – Skin Pigment Changes – Loss of Fatty Tissue – Tendon Rupture Instructions – Apply an ice pack to the injection site twice (2x) daily for 20 to 30 minutes. – Take anti-inflammatory medication or pain medications if you need something for injection site soreness. – Limit activities for at least 24 hours to minimize increased injection site pain and to maximize the benefits of the steroid medication. – If you have hives, rashes, difficulty breathing, facial swelling or anaphylactic symptoms, go to the closest Emergency Room or call 911 IMMEDIATELY. – If you get a red, swollen knee or run a fever >101.5ºF for 24 hours after the injection, call our office at 000-000-0000 or go to the Emergency Room. – If you experience a flare reaction call our office or the on-call provider at XXX-XXX-XXXX – Your follow up appointment will be on (date)____________- at ____________AM/PM |
5. Specific Injection Techniques for Common Musculoskeletal Conditions
Different musculoskeletal conditions require specific injection techniques to ensure accurate medication delivery and optimal outcomes. This section provides an overview of injection techniques for subacromial impingement syndrome, lateral epicondylitis, olecranon and prepatellar bursitis, ganglion cyst, trochanteric bursitis, and knee injection and aspiration.
5.1 Subacromial Impingement Syndrome
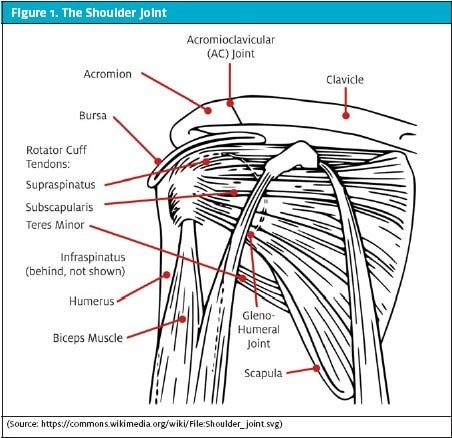
Subacromial impingement syndrome, also known as shoulder impingement, occurs when the tendons of the rotator cuff become compressed under the acromion. Corticosteroid injections into the subacromial space can help reduce inflammation and alleviate pain.
 Subacromial Injection
Subacromial Injection
- Patient Position: Seated with the arm relaxed.
- Landmarks: Coracoid process and acromial spine.
- Needle Insertion: Posterior approach, angling slightly cephalad.
5.2 Lateral Epicondylitis
Lateral epicondylitis, or tennis elbow, is an inflammation of the tendons that attach to the lateral epicondyle of the humerus. Corticosteroid injections can provide pain relief and promote healing.
- Patient Position: Seated with the elbow extended.
- Landmarks: Lateral epicondyle.
- Needle Insertion: Direct injection into the point of maximal tenderness.
5.3 Olecranon and Prepatellar Bursitis
Olecranon bursitis is an inflammation of the bursa located over the olecranon process of the elbow, while prepatellar bursitis affects the bursa in front of the kneecap. Aspiration of fluid and corticosteroid injection can reduce inflammation and relieve pain.
- Patient Position: Elbow or knee extended.
- Landmarks: Olecranon process or patella.
- Needle Insertion: Direct aspiration of fluid followed by corticosteroid injection.
5.4 Ganglion Cyst
A ganglion cyst is a fluid-filled sac that typically develops on the wrist or hand. Aspiration of the cyst and corticosteroid injection can provide temporary relief.
- Patient Position: Wrist or hand supported.
- Landmarks: Ganglion cyst.
- Needle Insertion: Direct aspiration of fluid followed by corticosteroid injection.
5.5 Trochanteric Bursitis
Trochanteric bursitis is an inflammation of the bursa located over the greater trochanter of the femur. Corticosteroid injections can reduce pain and improve mobility.
- Patient Position: Lateral decubitus position with the affected hip up.
- Landmarks: Greater trochanter.
- Needle Insertion: Direct injection into the point of maximal tenderness.
5.6 Knee Injection and Aspiration
Knee injections and aspirations are common procedures for managing knee pain and effusion. Corticosteroid injections can reduce inflammation, while aspiration can relieve pressure and provide fluid for analysis.
- Patient Position: Supine with the knee extended or slightly flexed.
- Landmarks: Patella and patellar tendon.
- Needle Insertion: Suprapatellar or infrapatellar approach.
6. Potential Risks and Complications of Joint and Soft Tissue Injections
While joint and soft tissue injections are generally safe and effective, they are not without potential risks and complications. Healthcare providers should be aware of these risks and take appropriate measures to minimize them.
6.1 Infection
Infection is a rare but serious complication of joint and soft tissue injections. Sterile technique is essential to prevent infection. Patients should be educated about the signs and symptoms of infection, such as redness, swelling, and fever, and instructed to seek medical attention if they develop these symptoms.
6.2 Bleeding
Bleeding can occur at the injection site, particularly in patients who are taking anticoagulant medications. Applying pressure to the injection site after the procedure can help minimize bleeding.
6.3 Nerve Injury
Nerve injury is a rare but potentially debilitating complication. Healthcare providers should have a thorough understanding of musculoskeletal anatomy to avoid inadvertent nerve damage.
6.4 Tendon Rupture
Repeated corticosteroid injections can weaken tendons and increase the risk of rupture. Limiting the frequency of injections and advising patients to avoid overuse can help prevent this complication.
6.5 Cartilage Damage
Corticosteroids can have toxic effects on cartilage, leading to degenerative changes in joint tissues. Healthcare providers should use the lowest effective dose and limit the frequency of injections to minimize this risk.
7. The Role of Imaging Guidance in Joint and Soft Tissue Injections
Imaging guidance, such as ultrasound or fluoroscopy, can enhance the accuracy and safety of joint and soft tissue injections. It allows healthcare providers to visualize the target structure and ensure accurate needle placement.
7.1 Ultrasound Guidance
Ultrasound guidance is a non-invasive imaging technique that uses sound waves to create real-time images of soft tissues and joints. It can be used to guide needle placement during injections and aspirations.
7.2 Fluoroscopy Guidance
Fluoroscopy guidance uses X-rays to create real-time images of bones and joints. It is particularly useful for guiding injections into deep or complex joints.
7.3 Benefits of Imaging Guidance
- Improved Accuracy: Imaging guidance can improve the accuracy of needle placement, particularly in difficult-to-access joints.
- Reduced Risk of Complications: By visualizing the target structure, imaging guidance can help reduce the risk of nerve injury and other complications.
- Enhanced Patient Comfort: Accurate needle placement can minimize pain and discomfort during the procedure.
8. Continuing Education and Training in Injection Techniques
Proficiency in joint and soft tissue injection techniques requires ongoing education and training. Healthcare providers should participate in continuing education courses and workshops to stay up-to-date on the latest techniques and best practices.
8.1 Anatomy Workshops
Anatomy workshops provide a hands-on opportunity to review musculoskeletal anatomy and practice injection techniques on cadaver specimens.
8.2 Ultrasound Training Courses
Ultrasound training courses teach healthcare providers how to use ultrasound to guide joint and soft tissue injections.
8.3 Online Resources
Online resources, such as webinars and instructional videos, can supplement formal training and provide ongoing learning opportunities. CONDUCT.EDU.VN offers a wealth of information and resources on joint and soft tissue injection techniques.
9. Ethical Considerations in Joint and Soft Tissue Injections
Ethical considerations play a crucial role in the practice of joint and soft tissue injections. Healthcare providers should adhere to ethical principles such as beneficence, non-maleficence, autonomy, and justice.
9.1 Informed Consent
Patients should be fully informed about the benefits and risks of joint and soft tissue injections before giving their consent. They should have the opportunity to ask questions and make informed decisions about their treatment.
9.2 Appropriate Indications
Joint and soft tissue injections should be used for appropriate indications, based on clinical evidence and best practices. They should not be used solely for patient convenience or financial gain.
9.3 Transparency and Honesty
Healthcare providers should be transparent and honest with patients about the expected outcomes of joint and soft tissue injections. They should not make unrealistic promises or guarantees.
10. Frequently Asked Questions (FAQ) About Joint and Soft Tissue Injections
This section addresses common questions about joint and soft tissue injections to provide clear and concise information for patients and healthcare providers.
10.1 What are joint and soft tissue injections?
Joint and soft tissue injections involve injecting medications, such as corticosteroids or local anesthetics, directly into joints or soft tissues to reduce pain and inflammation.
10.2 What conditions can be treated with these injections?
These injections can treat various musculoskeletal conditions, including arthritis, bursitis, tendonitis, and nerve impingement.
10.3 How effective are these injections?
The effectiveness of these injections varies depending on the condition being treated and individual patient factors. Many patients experience significant pain relief and improved function.
10.4 What are the potential side effects?
Potential side effects include infection, bleeding, nerve injury, tendon rupture, and cartilage damage. However, these complications are rare when proper technique and precautions are followed.
10.5 How often can I receive these injections?
To minimize the risk of side effects, it is generally recommended to limit the frequency of injections to no more than one injection every three to four months.
10.6 Are these injections painful?
The injection process may cause some discomfort, but local anesthetics are often used to minimize pain.
10.7 How long does it take for the injection to work?
The onset of pain relief varies depending on the medication used. Local anesthetics provide immediate relief, while corticosteroids may take a few days to take effect.
10.8 How long does the pain relief last?
The duration of pain relief varies depending on the individual and the condition being treated. Some patients experience relief for several months, while others may require repeat injections.
10.9 Can these injections cure my condition?
These injections are primarily used to manage pain and inflammation. They may not cure the underlying condition, but they can provide significant symptom relief.
10.10 Are there any alternatives to these injections?
Alternatives to these injections include physical therapy, oral medications, and surgery. The most appropriate treatment option depends on the individual and the condition being treated.
Conclusion: Enhancing Musculoskeletal Care Through Expertise
Mastering the art and science of joint and soft tissue injections demands a steadfast commitment to continuous learning, meticulous technique, and ethical practice. The comprehensive guidance provided by CONDUCT.EDU.VN aims to empower healthcare professionals with the knowledge and skills necessary to deliver safe and effective musculoskeletal care. By staying informed and adhering to best practices, practitioners can optimize patient outcomes and improve the quality of life for individuals suffering from musculoskeletal conditions.
For more detailed information and expert guidance on joint and soft tissue injections, visit conduct.edu.vn. Our resources include in-depth articles, instructional videos, and continuing education opportunities to enhance your proficiency in musculoskeletal care. Contact us at 100 Ethics Plaza, Guideline City, CA 90210, United States or Whatsapp: +1 (707) 555-1234.
